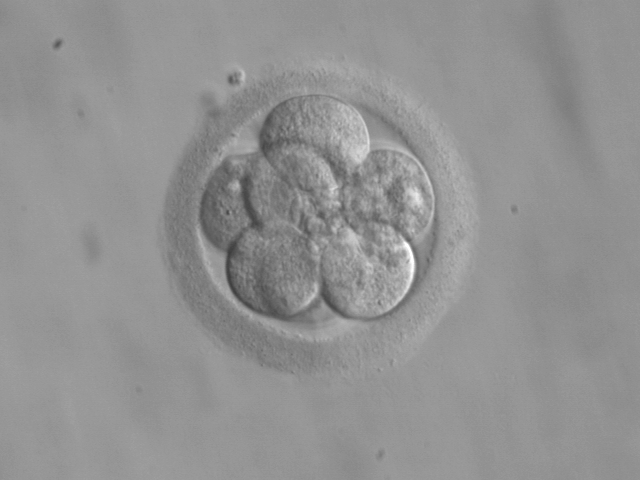
Changes to ethics guidelines allow scientists to take a closer look at our beginnings
Scientists know quite a bit about 3-day-old human embryos like the one pictured. But they don’t have a clear picture of how human embryos develop between Days 14 and 28. (Credit: ekem, courtesy Robert Wood Johnson Medical School IVF Program, Wikimedia Commons)
“Model embryos” created from stem cells may illuminate the black box of early human development
Recent changes to guidelines that restrict how long scientists can grow human embryos in a laboratory could lead to a clearer understanding of genetic abnormalities and diseases.
The changes will also allow researchers to learn more about a crucial period in human development, said molecular biologist Ali Brivanlou, who heads the Laboratory of Synthetic Embryology at Rockefeller University. He spoke Oct. 8 during the Council for the Advancement of Science Writing’s Perlman Symposium at the virtual ScienceWriters2021 conference.
The International Society for Stem Cell Research, or ISSCR, sets ethics guidelines for scientists. Although countries are free to make their own laws—or not—in accordance with society, researchers have generally abided by the longstanding guidelines, including the “14-day rule,” which prohibits growing a human embryo in a laboratory beyond 14 days.
Until a few years ago, the 14-day rule was mostly theoretical; the technology didn’t exist to keep an embryo alive and growing in the laboratory for much more than that. The ISSCR decided this year to reexamine the rule, allowing experiments involving human embryos to go beyond 14 days on a case-by-case basis. Experiments are subject to several phases of review and approval to determine at what point they must be stopped.
There are compelling reasons to look beyond the 14-day window, Brivanlou said.
At Day 14, cells start to differentiate in the embryo, determining what will be top and bottom, left and right. Days 14 through 28 see the beginnings of the central nervous system, heart and other organs. This is also the time that many things can go wrong: genetic abnormalities, disease, and miscarriage. But this interval is a “black box” about which researchers know very little. Studying this crucial period could lead to a better understanding of these problems and possible treatments.
The previous, more restrictive guidelines prevented Brivanlou from continuing promising research. Several years ago, his team discovered that new types of cells that could become organs had begun forming in a human embryo. But they stopped the work on Day 13 out of respect for the guidelines.
“It was one of the toughest decisions I’ve made in my life. And I can assure you I’ve had a lot of tough ones to make,” he said. “We have no idea right now what this organ is…. It’s mind-blowing to realize that we don’t even know our anatomy … before birth, at the very early stages.”
The updated ethics guidelines will aid not just human embryo research, but also the development of models based on stem cells that can substitute for the real thing. Stem cells have the potential to become nearly any type of cell in the human body. Researchers such as Brivanlou can guide these stem cells to mimic phases of early human development, allowing study without the same ethics concerns as culturing a human embryo.
The stem cell models ultimately have to be validated against human embryos, some of which might be past 14 days, to demonstrate that they are good substitutes. These new capabilities could point scientists in surprising directions.
For example, Brivanlou’s lab recently used model embryos to show that neurodegenerative diseases such as Huntington’s originate during the first few weeks of human development. Model embryos could also be used to screen drugs, with more accurate models yielding better-targeted therapies.
Brivanlou anticipates that progress will be made in culturing embryos and validating stem cell models alongside continued careful attention to the ethics issues involved. “We really want to reconcile the scientific world with ethical and moral, social political values in the society in which we’re operating.”